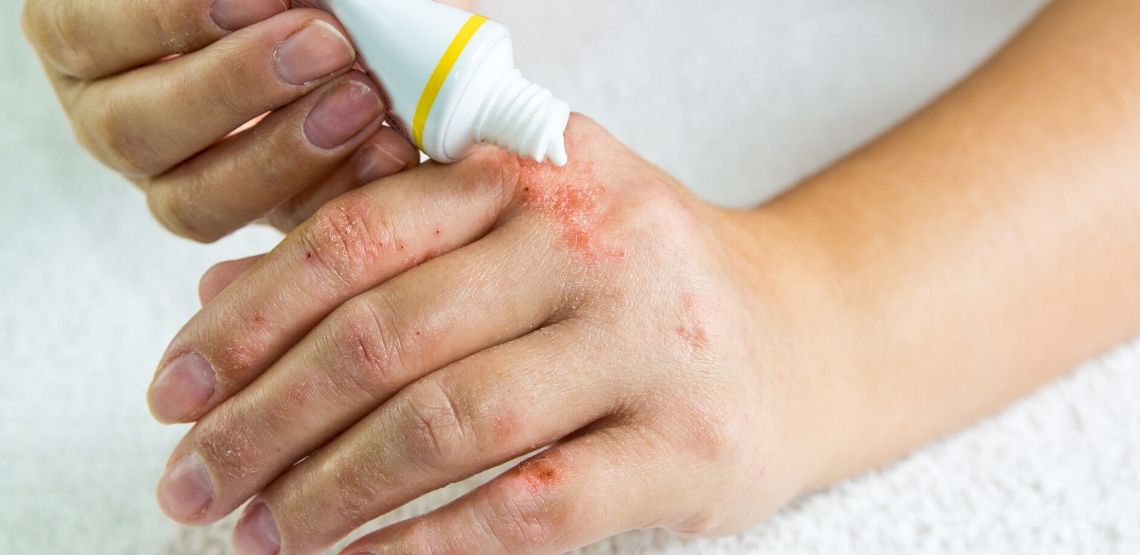
What is Eczema?
Eczema is an inflammatory condition of the skin that causes patches of redness, itching and sometimes pain. In this article, we discuss everything you need to know about eczema, including its symptoms, causes and treatment options.
Symptoms
The symptoms of eczema can range from mild to extremely severe. They may affect small, isolated parts of the body or be more widespread, covering large areas of skin.
The most common eczema symptoms include:
- Dry or scaly skin.
- Itching.
- Redness.
- Soreness.
- Cracking.
- Bleeding.
Although the condition is not an infectious disease (it cannot be passed onto others), it can increase the risk of infections in the affected areas. Skin infections may require treatment with antibiotics. Therefore, you should see your physician if any of the following symptoms occur:
- Worsening of normal symptoms.
- Weeping or oozing skin.
- Yellow crusty patches or yellow spots.
- Swelling.
- Pain or soreness.
- Fever.
Symptoms can come and go over time. Some people who develop the condition during childhood find that their symptoms improve by the time they reach adulthood. However, some people experience eczema flare-ups throughout their lives.
The Different Types of Eczema
There are many different types of eczema and they all have slightly different symptoms:
- Contact dermatitis is a type which is triggered by exposure to a particular substance. The immune system recognizes this substance as a threat, triggering an inflammatory response.
- Dyshidrotic eczema is a type which causes blisters to form on the palms of the hands and soles of the feet.
- Nummular eczema, also known as discoid eczema, causes circular patches of inflamed skin. These can become itchy, scaly and crusty.
- Stasis eczema, also known as varicose eczema, tends to occur on the lower legs. It is the result of a circulatory problem.
- Neurodermatitis is a type of eczema which causes scaly patches on the head, forearms and lower legs. It can be extremely itchy.
- Seborrheic eczema tends to affect the scalp. It can cause itchy, scaly patches and dandruff.
However, the most common type by far is atopic eczema. When people talk about eczema, they are usually referring to this particular form of the condition.
Related Search Topics (Ads)
What Causes Eczema?
Atopic eczema tends to occur in people whose immune systems are overly sensitive. These patients often suffer from conditions like asthma and allergies alongside their eczema. It often runs in families and genetics is one of the biggest risk factors.
Some possible causes of flare-ups include:
- Using products which irritate the skin (detergents, toiletries).
- Wool clothing or synthetic fibers.
- Food intolerances.
- Stress.
- Cold or damp weather.
- Excessive sweating.
- Hormones (many women find their eczema changes throughout their menstrual cycle).
One of the best ways to manage the symptoms is to identify any triggers and avoid them as much as possible.
Eczema Treatment Options
There is currently no cure for eczema, but there are several treatment options which can help manage symptoms.
Emollients
Emollients are products which are designed to lock moisture into the skin. They come in the form of ointments, creams and lotions.
Ointments are the greasiest and are suitable for areas of very dry skin. Lotions are the least greasy and are suitable for applying to larger areas. Creams are somewhere in between the two. Some emollients can also be added to bath water or used as a soap substitute.
It is essential that anybody with eczema applies an emollient several times a day, even when they are not experiencing symptoms. They help to prevent dryness, itching and keep eczema symptoms at bay.
Corticosteroids
Corticosteroids, such as hydrocortisone, are available as creams and ointments which can be applied to inflamed skin. They should only be used for short periods as long-term use can increase the risk of side effects, including thinning skin, changes in skin color, acne and increased hair growth.
The best time to apply corticosteroids is at least 30 minutes after applying emollient, or at a different time of day. Continue use for 48 hours after the symptoms clear to tackle any residual inflammation.
Oral corticosteroids are also available, but doctors usually only prescribe these in extreme cases.
Calcineurin Inhibitors
Drugs such as pimecrolimus and tacrolimus may be useful if other treatments have not been effective. They work by inhibiting activity in the immune system.
Antihistamines
Some people use antihistamines to reduce the itching. They may cause drowsiness and are especially helpful for people whose itching keeps them awake at night. However, they should be used with caution by anyone who is driving or operating machinery.
Phototherapy
If other treatments have failed, your dermatologist may recommend phototherapy. This treatment uses UVA and UVB rays to relieve the symptoms.
Natural Remedies
Some patients find natural remedies for eczema helpful. These include herbal medicines and treatments such as acupuncture. However, there is limited evidence to support their use.
Living With the Skin Condition
In addition to the above treatments, there are several steps that patients can take to reduce the risk of flare-ups. These include the following:
- Bathe in lukewarm water and apply an emollient immediately afterwards.
- Use a towel to gently pat yourself dry rather than rubbing vigorously.
- Try to resist scratching itchy skin and rub it gently instead.
- Keep fingernails short.
- Wear cotton gloves at night to prevent scratching.
- Identify and avoid any triggers (detergents, soap, foods).
By making these simple changes and applying emollient frequently, it is usually possible to manage symptoms naturally and reduce the need for further treatment.