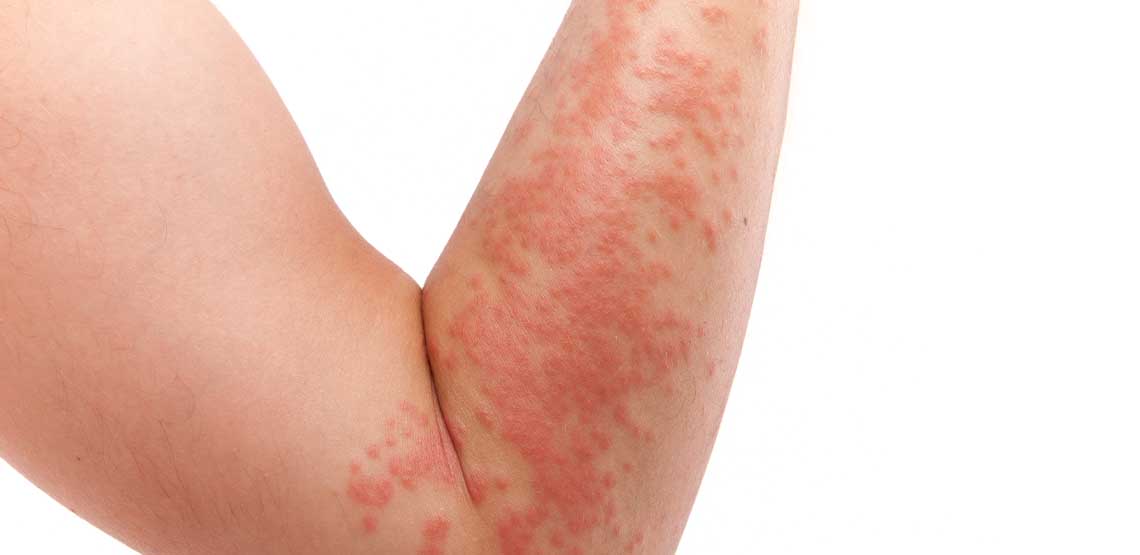
What Is Psoriasis?
Psoriasis is a disorder that accelerates the normal growth rate of skin, causing the skin to multiply as much as 10 times faster than normal.
In healthy, normal skin without psoriasis, skin cells naturally shed and flake off as the skin grows and multiples. But because the skin’s growth rate is so sped up in people with psoriasis, the skin accumulates and piles up before it has a chance to shed. Because of this, the skin can become inflamed and red, taking on a bumpy, scaly texture in patches.
These areas are known as plaques and are sometimes painless though unsightly for some. In some cases, they itch, burn or sting. They can crack and bleed, and in severe cases, they can expand to cover very large swaths of skin.
Theses plaques can appear anywhere on the body but typically crop up on the knees, elbows, scalp, or lower back. In addition, the effects of psoriasis can be seen in the discoloration and crumbling of fingernails and toenails (though this doesn’t affect all of those with psoriasis.)
It’s likely you know someone living with psoriasis, if not several people. In fact, it’s very common, affecting at least 8 million Americans. Psoriasis doesn’t discriminate and can show up later in life or on children – though it’s typical for it to first rear its head in early adulthood. Psoriasis can also affect people of any gender, race, or ethnicity.
How Do You Get Psoriasis?
Psoriasis is an inflammatory disease and it occurs because of an overactive immune system. Because of this, the affects can go beyond just the visible irritation of the skin. If left untreated, the effects of psoriasis can make their way into the body’s joints, creating psoriatic arthritis. It’s estimated that between around 30% of those with psoriasis will develop the accompanying swelling and arthritis of the joints. For this reason, it’s crucial to diagnose and treat psoriasis before it does any lasting damage
How do you get psoriasis? The disease can seem quite mysterious and frustrating to understand and treat, especially because it’s something that can appear later in life, seemingly without any clear cause.
Unfortunately, scientists still aren’t 100% clear on what exactly triggers the development of psoriasis, only that it has to do with the immune system in general, and for this reason, can be triggered by a plethora of factors or a combination thereof.
There are some common causes:
- Emotional stress
- Surgery
- Medications, such as blood pressure medications or hydroxychloroquine
- Strep infections
- Cuts or scrapes or any minor injury to the skin like bug bites or sunburn
Related Search Topics (Ads)
Keep in Mind…
It’s important to note that the causes or triggers of psoriasis vary widely from person-to-person and are still not entirely understood. However, stress tends to be one of the most common triggers. Less common but still possible triggers for psoriasis include environmental factors or even food allergies or alcohol.
Also, worth noting, there’s an element of genetics that pay into the likelihood of developing this condition, meaning that if you have an immediate family member with the condition, you’re more likely to develop it yourself. Interestingly, it’s also been known to skip a generation, so it’s possible your parents didn’t have it but a grandparent may have.
It’s also very important to know that despite the slight air of mystery surrounding the origins, it is known for sure that it’s not contagious from person-to-person. If you shake hands or otherwise contact someone with psoriasis, there is no need for concern that you’ll get it.
Prevention Tips and Early Signs to Look Out For
In many cases, it can emerge for the first time with little if any warning, and often appears on those between the ages of 15 to 25 (but it can pop up at any age.)
The signs and early symptoms, like the disease itself, vary. Typically, they’ll manifest as patches of the telltale red, scaly, inflamed skin. The scales themselves often are described as having a silver color to them. Itchy skin that cracks and bleeds can also be psoriasis. The areas of inflammation can be small or widespread and on various areas of the body – the scalp is common though. You may also notice issues with your fingernails and/or toenails.
If you suspect your red, itchy, bumpy skin may be psoriasis, see your doctor or a dermatologist. In most cases, they can diagnose it on sight by doing a simple and painless physical exam, or if needed, they can go more in depth with a skin biopsy test.
Once they’ve diagnosed your skin condition, your health care provider can prescribe you with one of the many treatment options available (including topical ointments and medications) for controlling and improving your skin’s health. Luckily, living with psoriasis is not just possible but common and very doable, and there are any treatment options that can be used to find relief.